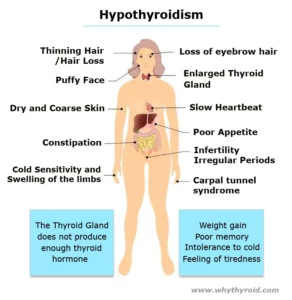
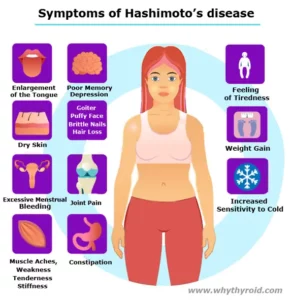
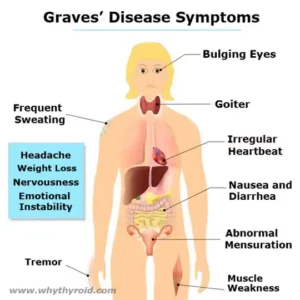
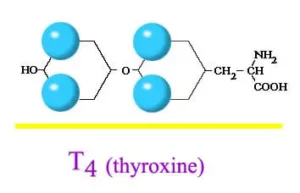
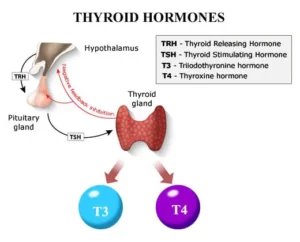
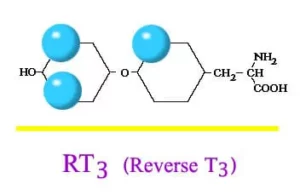
Levothyroxine is a medicine used to treat hypothyroidism. If you have hypothyroidism, it means your thyroid gland produce too little thyroid hormone. With low thyroid hormone levels, your body cannot function properly, which may result in poor growth, lack of energy, excessive tiredness, weight gain, hair loss, increased sensitivity to cold, joint and muscle pain, heavy or irregular menstrual periods, and depression.
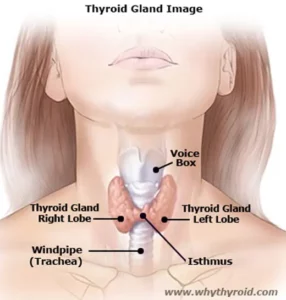
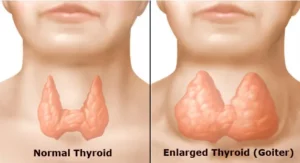
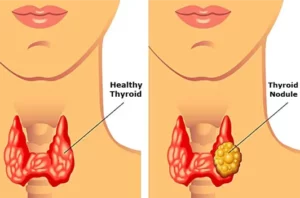
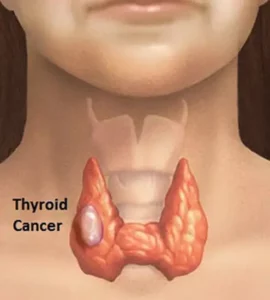
When taken correctly, levothyroxine provides thyroid hormone to you and restores the balance of thyroid hormone in your body. In addition, levothyroxine also can be used to treat goiter, which is an enlarged thyroid gland. It also treats certain types of thyroid cancer.
|
Important Warning
|
|
1. Levothyroxine, should not be used to treat weight loss or to treat obesity.
|
|
2. Levothyroxine may cause serious or life-threatening problems when taken higher than recommended doses. Therefore, never take more than the prescribed dose.
|
|
3. Levothyroxine is only available on prescription.
|
|
4. Please talk to your doctor before you start taking levothyroxine.
|
Continue reading…