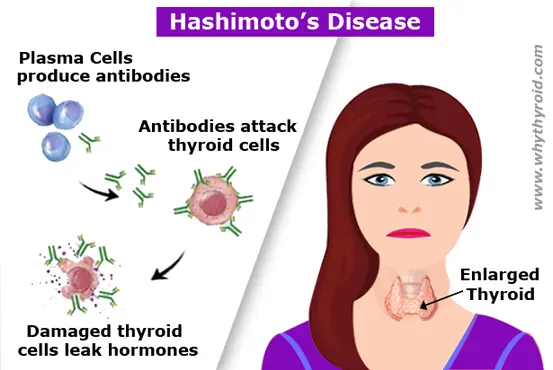
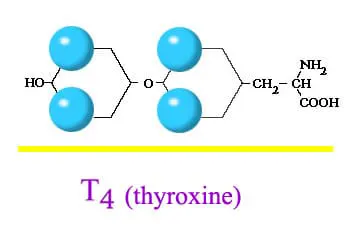
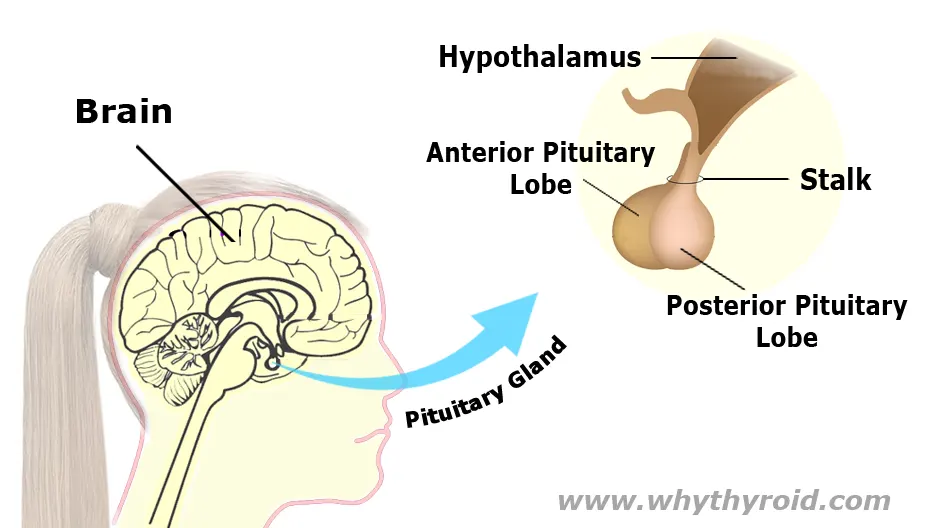
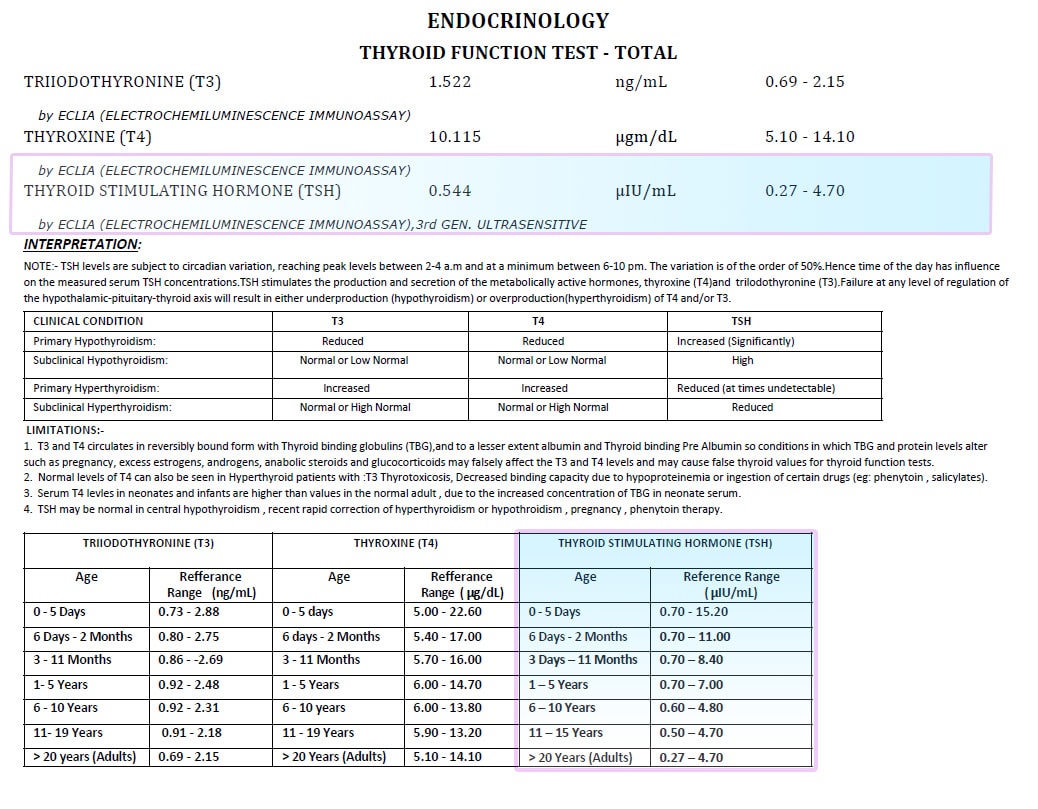
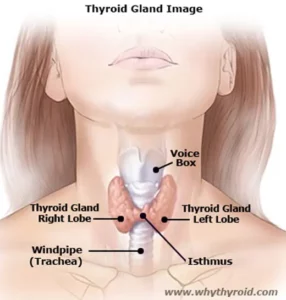
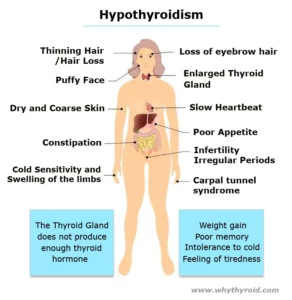
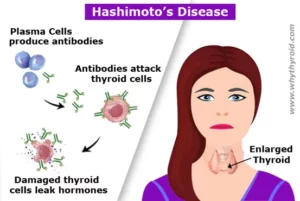
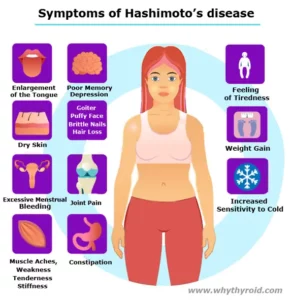
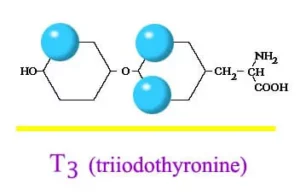
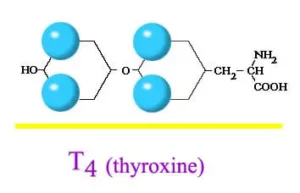
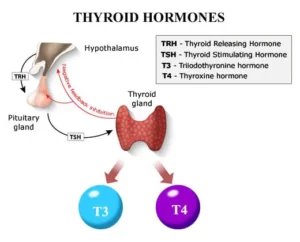
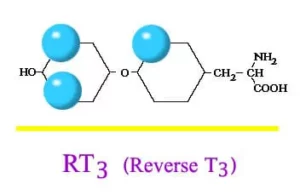
Hashimoto’s Disease is an autoimmune disorder in which the immune system mistakenly attacks the thyroid gland. This can lead to hypothyroidism, a condition in which thyroid does not make enough hormones for body’s need. Hashimoto is the most common cause of hypothyroidism (an underactive thyroid).
Generally immune system protects body against bacteria and viruses. But in Hashimoto’s Disease, immune system make antibodies, which attacks the cells of thyroid gland. Doctors do not know why this happens, but some scientists believe genetic factors may be involved. The disease affects more women than men.
Continue reading…