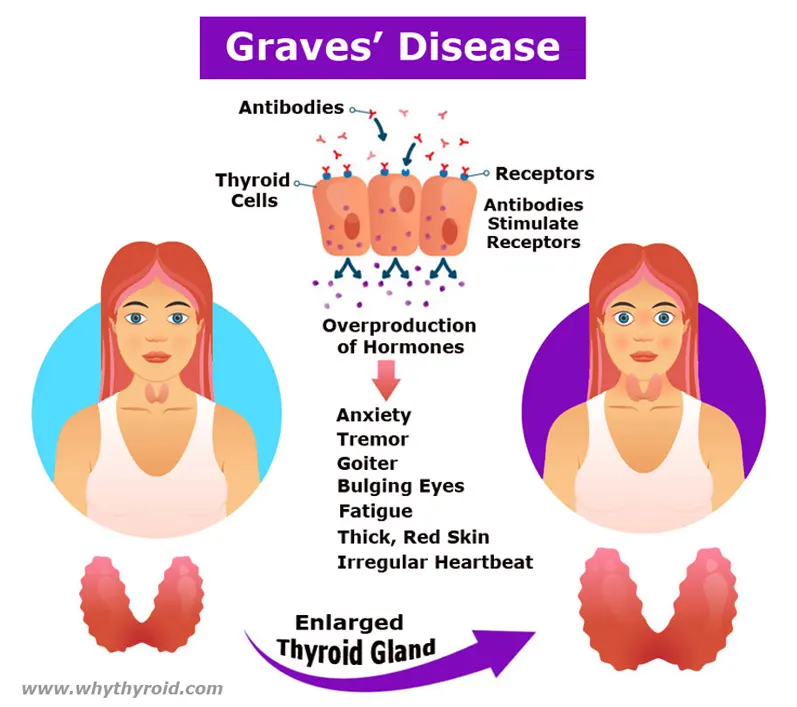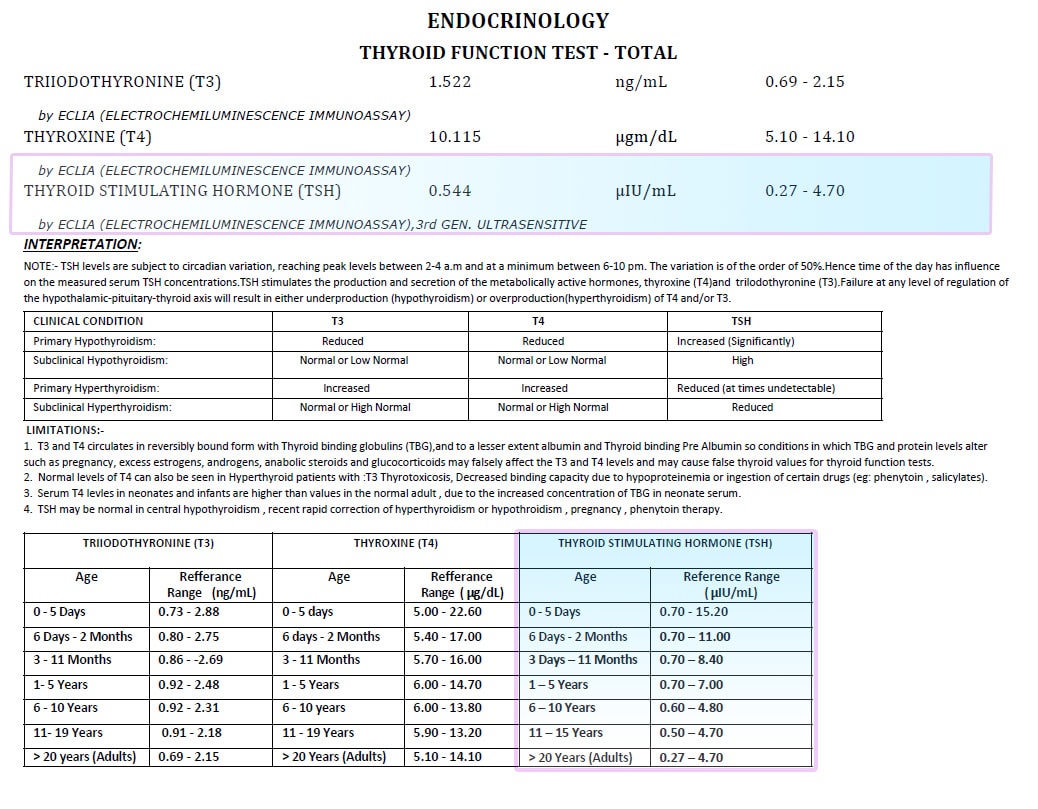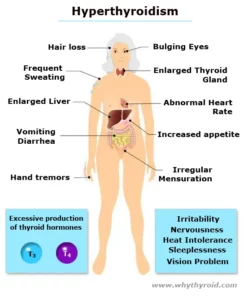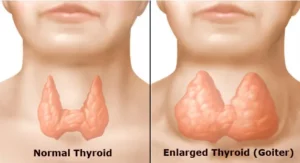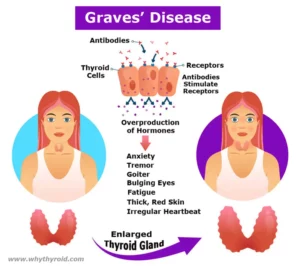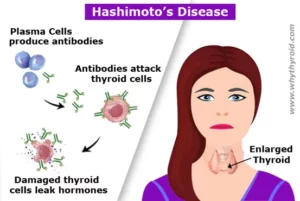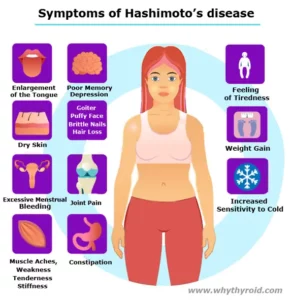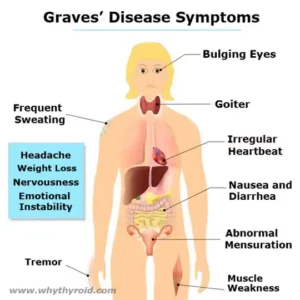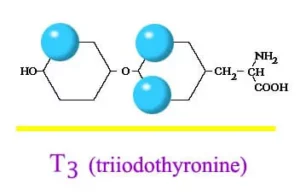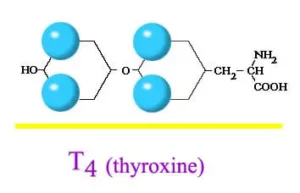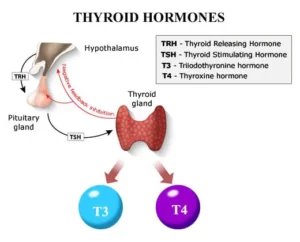
Antithyroid medications are used to treat an overactive thyroid gland (also know as hyperthyroidism). When the thyroid gland is overactive, it makes too much thyroxine (also known as T4). The extra thyroxine can accelerate the metabolism rate of your body. As a result, it can cause weight loss and irregular heart activity.
Therefore, antithyroid medications (which includes methimazole and propylithiouracil) are used to reduce the amount of hormone (T4) released by the thyroid gland. These drugs does not affect the thyroxine which is already made, but reduce the further production. Therefore, it may take four to eight weeks of treatment for your thyroxine level to come down to normal.
Continue reading…