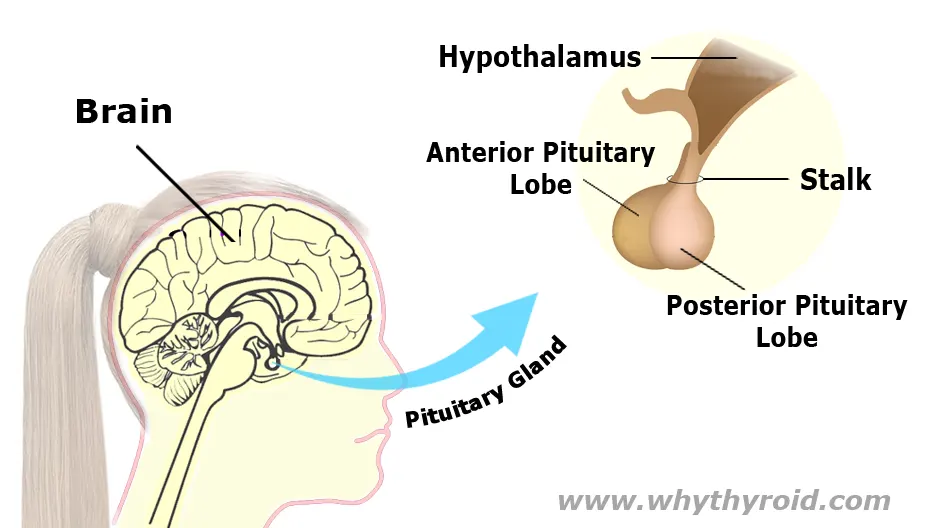
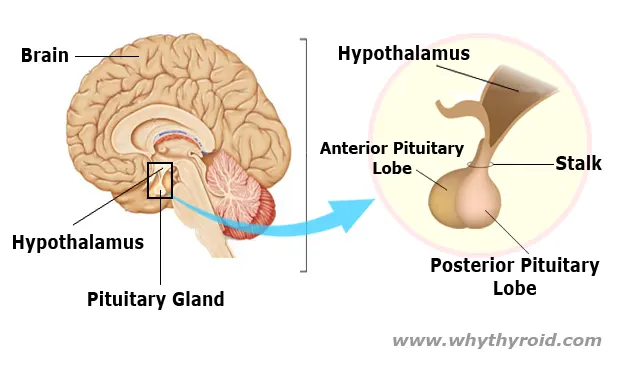
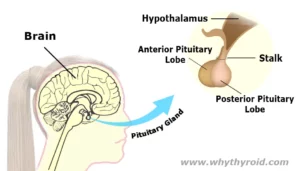
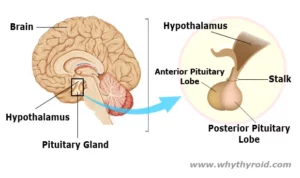
Your Pituitary gland is the main endocrine (hormone producing) gland that sits just beneath the base of the brain. It is very small in size (only about the size of a pea).
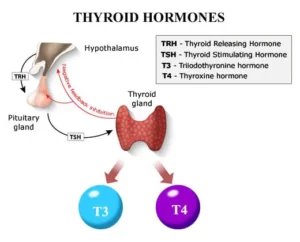
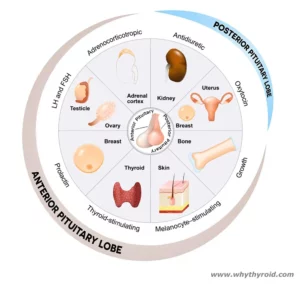
It produces hormones that controls the function of many other hormone glands in your body (especially the thyroid, adrenals, ovaries and testicles). Therefore, the pituitary gland is often called the master gland of the endocrine system.
Continue reading…