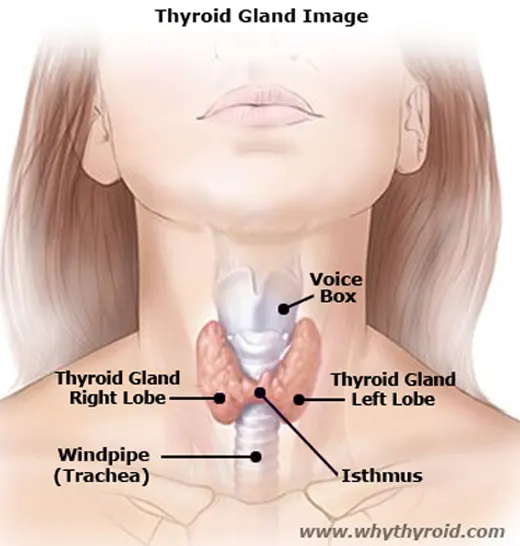
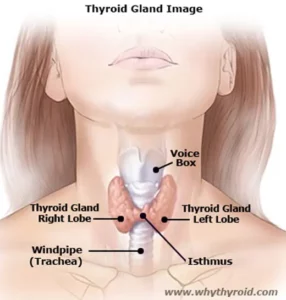
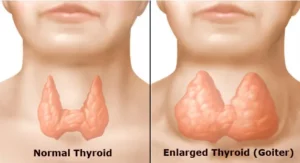
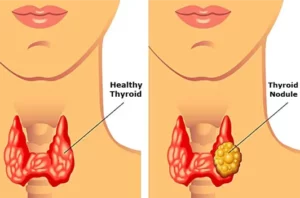
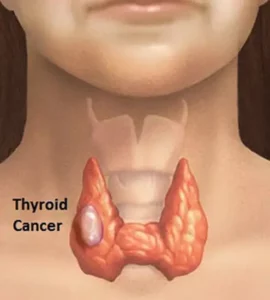
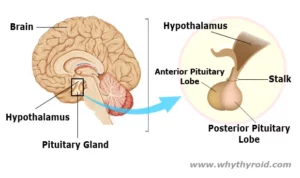
Thyroid is a small gland (about 2 inches long) which has the shape like a butterfly that lies in the front of your neck. It has two sides called lobes, located either side of your windpipe. Further, these two lobes of the gland are connected by a small tissue called the isthmus.
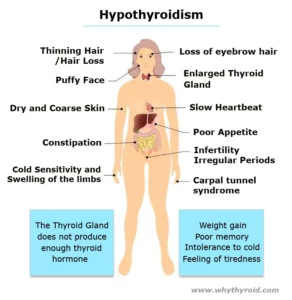
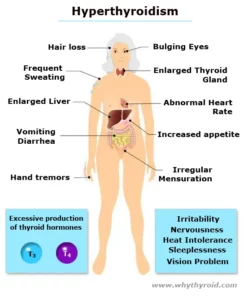
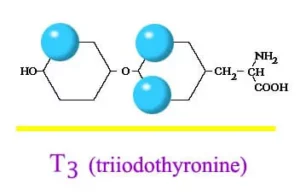
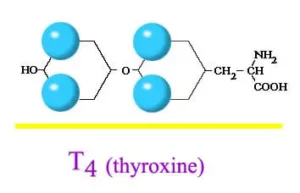
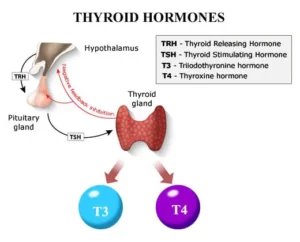
Thyroid is a vital hormone gland which plays a major role in metabolism, growth, development, temperature, weight and heart rate of the human body by constantly releasing a steady amount of thyroid hormones (T3 and T4) into the bloodstream. Also, during infancy and childhood, adequate thyroid hormone is crucial for brain development.
Continue reading…